Vasculitis
This rare disorder causes the immune system to attack blood vessels.
Vasculitis is an autoimmune disease that causes inflammation and narrowing of blood vessels (arteries, veins and capillaries). These vessels carry blood to and from the heart and the body’s organs.
In severe cases, the condition can cause organ damage or death.
Types of vasculitis are grouped according to the size of the blood vessels affected. Most types of vasculitis are rare and include:
- Large vessel – Polymyalgia rheumatic, Takayasu's arteritis, temporal arteritis (giant cell arteritis)
- Medium vessel – Buerger's disease, cutaneous vasculitis, Kawasaki disease, polyarteritis nodosa
- Small vessel – Behçet's syndrome, Churg-Strauss syndrome, cutaneous vasculitis, Henoch-Schönlein purpura, microscopic polyangiitis, granulomatosis with polyangiitis, Golfer's vasculitis, cryoglobulinemia
Vasculitis symptoms may occur once or several times over several years. The disease affects people of all ages, races and gender.
Causes
Vasculitis occurs when the immune system mistakenly sees blood vessels as a foreign invader and attacks them. What causes this to happen isn't fully understood. These conditions can occur by themselves or with other rheumatic diseases, such as rheumatoid arthritis, systemic lupus erythematosus (SLE/ lupus) or Sjogrens syndrome. Other possible triggers include an infection (hepatitis B or C) or a medication side effect. Vasculitis also may be linked to certain blood cancers, such as leukemia and lymphoma.
Symptoms
Signs and symptoms of vasculitis vary and can range from mild to life-threatening. They depend on the type of vasculitis, the organs involved and how severe the condition is. Some people may have few signs and symptoms. Other people may become very sick. Sometimes symptoms develop slowly, over months, while at other times, the signs and symptoms start quickly, over days or weeks.
Common symptoms include:
- Fever.
- Loss of appetite.
- Weight loss.
- Fatigue.
- General aches and pains.
Vasculitis can affect organs and body systems, causing a range of signs and symptoms including:
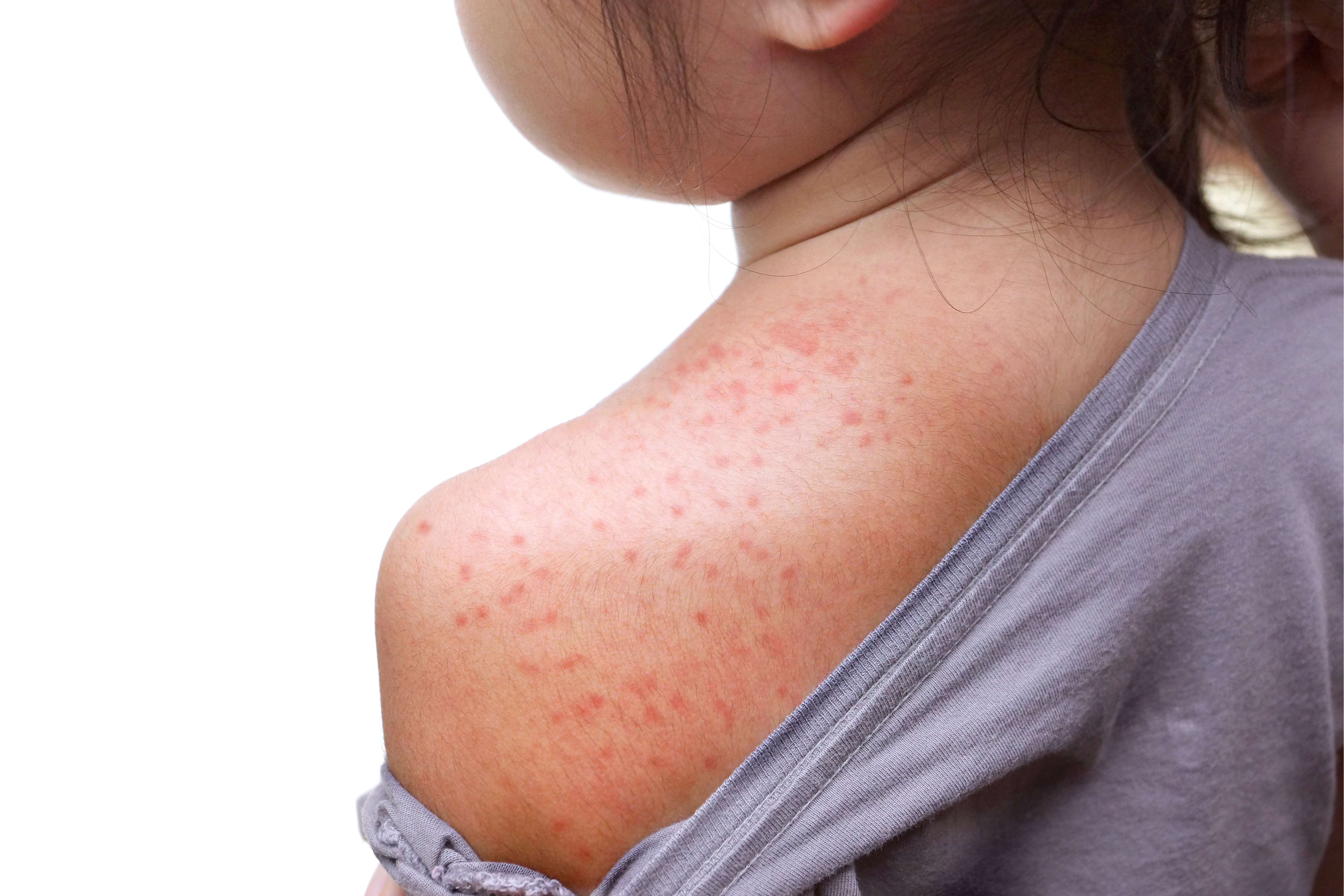
- Skin – purple or red spots or bumps; clusters of small dots, splotches, bruises, or hives; itching.
- Joints – aching or arthritis in one or more joints.
- Lungs – shortness of breath; coughing up blood.
- Gastrointestinal tract – sores in the mouth; stomach pain; in severe cases, blockage of blood flow to the intestines that can cause weakening or rupture of intestines.
- Sinuses, nose, throat and ears – sinus or chronic middle ear infections; sores in the nose; in some cases, hearing loss.
- Eyes – red, itchy, burning eyes; light sensitivity; blurred vision; rarely, blindness.
- Brain – headaches; problems thinking clearly; changes in mental function; stroke-like symptoms, such as muscle weakness and paralysis.
- Nerves – numbness, tingling and weakness in various parts of the body; loss of feeling or strength in hands and feet; shooting pains in arms and legs.
In severe cases, vasculitis can cause blood vessels to close off, so blood can’t flow through or they bulge and possibly burst (aneurysm).
Diagnosis
Vasculitis is diagnosed based on signs and symptoms, medical history, a physical exam and test results.
- Laboratory tests – blood and urine tests may show abnormal levels of certain blood cells and antibodies (proteins) in the blood.
- Biopsy – this is often the best way to make a firm diagnosis of vasculitis. During a biopsy, the doctor takes a small sample of an affected blood vessel or organ to study under a microscope, looking for signs of inflammation or tissue damage.
Other possible tests and examinations the doctor may perform will depend on the symptoms and may include:
- Angiography.
- Urinalysis.
- Echocardiogram.
- Chest X-ray.
- Lung function tests.
- Abdominal ultrasound.
- Computed tomography (CT) scan.
- Magnetic resonance imaging (MRI).
- Blood pressure measurement.
- Electrocardiogram (EKG).
Treatment
Treatment for vasculitis depends on the type of vasculitis, which organs are affected and the severity of the condition. The main goal of treating vasculitis is to reduce inflammation in the affected blood vessels. People who have severe vasculitis are treated with prescription medicines. People who have mild vasculitis may find relief with over-the-counter pain or anti-inflammatory medicines, such as acetaminophen, aspirin, ibuprofen or naproxen.
Common prescription medicines used to treat vasculitis include corticosteroids and disease-modifying antirheumatic drugs (DMARDs). Corticosteroids such as prednisone, prednisolone and methylprednisolone, help reduce inflammation in the blood vessels. Doctors may prescribe disease modifying anti-rheumatic drugs, such as azathioprine, methotrexate and cyclophosphamide, if vasculitis is severe or if corticosteroids don't work well. These drugs attack the source of inflammation
Self Care
In addition to closely following prescribed treatment, the following steps help to manage vasculitis:
- Eating a healthy diet.
- Getting routine vaccinations.
- Exercising regularly.
- Maintaining a strong support system.

Stay in the Know. Live in the Yes.
Get involved with the arthritis community. Tell us a little about yourself and, based on your interests, you’ll receive emails packed with the latest information and resources to live your best life and connect with others.